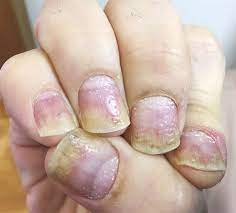
The most common nail changes
Psoriasis nail changes – one of the most common nail changes that occur with psoriasis.
They are characterized by:
● nail breakage
● indentation of the nail plate
● nail pits (the thimble phenomenon)
● a change in the color of the nail to yellow or brown (symptom of an oil stain)
● thickening of the skin under the nail
●separation of the nail plate from the base
Once these changes are detected, it is useful to investigate for a fungal nail infection, especially if the lesion is only visible in the toenails. In about 20% of cases, fungal nail infection can occur together with psoriatic nail changes.
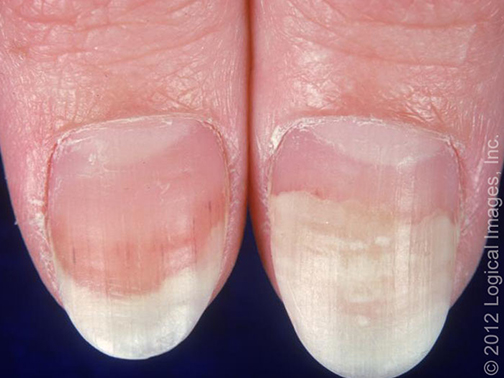
Onycholysis – separation of the rear or rear-lateral part of the nail plate from the base (bottom) and/or lateral structures of the nail.
A characteristic sign – the damaged part of the nail plate is white due to the air under the nail plate.
Onycholysis can be triggered by factors such as:
● trauma
● working in a wet environment
● psoriasis
● Lichen planus
● certain medications
● onychomycosis (fungal nail infection)
● allergic or contact dermatitis
With onycholysis, there is an increased tendency to contribute to secondary skin infection.
General measures to reduce onycholytic nail damage:
● Cut your nails short
● Avoid injuries
● Avoid contact with irritants
● Avoid humid environmental conditions
● Do not use nail cosmetics
● Protect hands from cold or windy weather
Paronychia – acute or chronic inflammation or infection of the skin around the edge of the nail (callus). It occurs much more strongly in people who have diabetes or immunosuppressive diseases.
Acute paronychia:
- lasts up to 6 weeks
- anyone can face:
-
-
- can start after a manicure
- common in young children who suck their fingers
- for people who bite their nails
- those taking retinoid therapy or other medications (retinoids dry out the skin)
- in the presence of ingrown nails
-
-
- causative agents: bacteria, viruses, fungi
- develops within a few hours, usually only one nail is affected
- main symptoms: pain, swelling of the skin around the nail, redness
- in the presence of the causative agent S. Pyogenes (of bacterial origin), it can appear together with fever, lymph node enlargement
- treatment depends on the causative agent, in rare cases surgical intervention, removal of the nail may be necessary
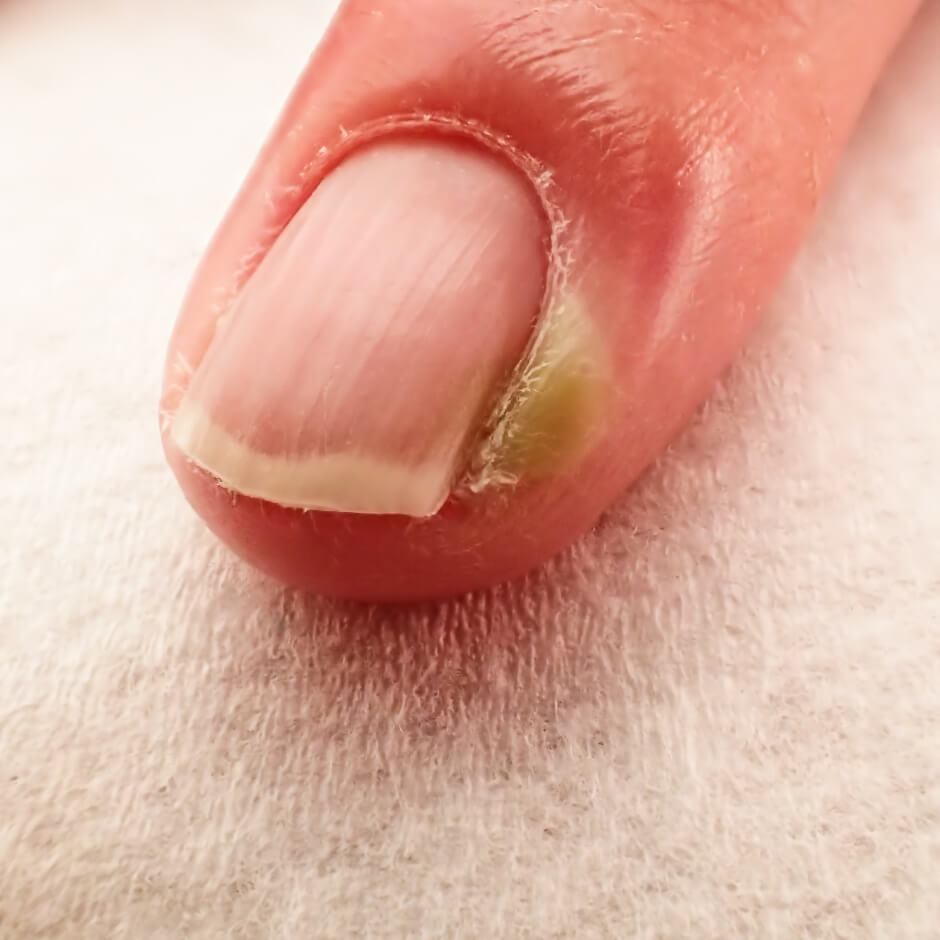
Chronic paronychia:
● lasts longer than 6 weeks
● characteristic of people with hand dermatitis who work in jobs where the hands are constantly exposed to cold and moisture
● it appears slowly, at the inner end of one nail, spreads along the sides of the nail, then passes to other nails
● the skin around damaged nails swells, the nail plate rises from the base, then it is easier for microorganisms and irritating substances to enter, which can cause inflammation and infection
● the affected skin may be reddened, more painful, and sometimes pus may appear
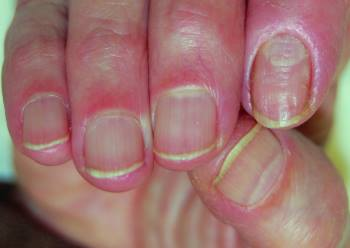
● the damaged nail becomes thinner, may be furrowed in horizontal lines
● treatment depends on the cause of the disease, it is important to remove environmental irritants, observe hand hygiene, apply moisturizing creams
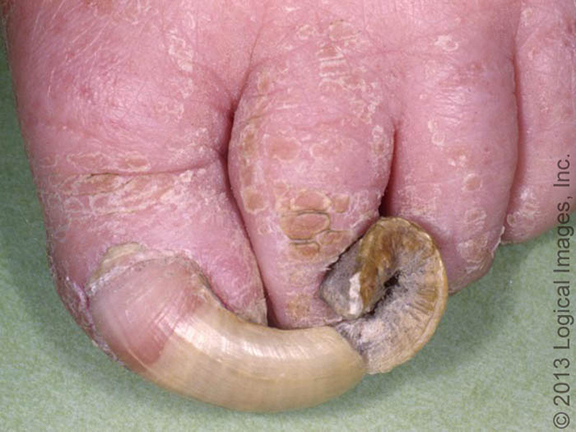
Onychogryposis (otherwise “ram’s horn nail”) – an acquired nail change, usually characteristic of the big toenail.
- The changed nail becomes:
-
- thickened
- yellowish brown
- longer and distorted
-
- It is characteristic of the elderly and persons who do not observe personal hygiene
- The cause of onychogryposis is not fully understood and may be related to peripheral vascular disease, repetitive trauma from tight-fitting footwear, and self-neglect
- Onychogryposis can be an expression of hereditary diseases (Apillon-Lefèvre syndrome, Haim-Munk syndrome and others)
- Possible complications: nail ingrowth, paronychia and secondary onychomycosis (fungal infection of the nail)
- Treatment with conservative measures (eg nail clipping/filing/grinding with nail clippers and electric clippers, use of appropriate footwear) may be an option.
- Surgical treatment – removal of the nail
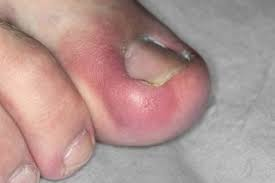
Ingrown nails – a nail condition that is characterized by redness and swelling of the skin around the ingrown nail and can lead to infection.
Heredity may play a role in this change, but other factors have also been identified:
- wearing tight, uncomfortable footwear
- long-term non-cutting of the nail
- injury to the nail
- wrong nail cutting
Ingrown nails are characterized by the surrounding skin:
- redness
- swelling
- soreness
- suppuration
Depending on the situation, the treatment may be surgical, pain medications may be used, you should also avoid humid environments, wear comfortable shoes, and cut your nails straight.
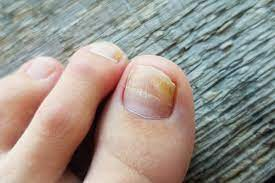
Onychomycosis – fungal infection of the nail, usually manifested by a change in the color of the nail, thickening and deformation of the nail.
This infection can be triggered by:
● sweating
● wearing inappropriate (pressing) footwear
● pedicures or manicures are performed in beauty salons
Is characterized by:
● a change in the color of the nail to yellow, brown or white
● nails that break easily
● thickened nails
● pain is usually not characteristic
For treatment, topical (medicated varnishes) or oral antifungal preparations are used.
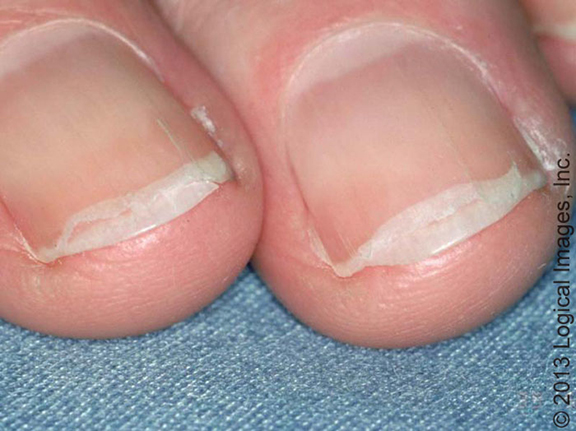
Onychoschisis (otherwise lamellar dystrophy) – a change in the nail characterized by lamellar separation of the free edge of the nail.
● It is often caused by external factors – work in a humid environment, chemicals affecting the nails, injuries
● Less often, iron deficiency, other chronic diseases
● The main symptom is easily broken nails. If only the nails of the hands are damaged, then the causes are external, if both the feet and hands are damaged, then the causes are internal
● Treatment is based on avoiding external irritants and using moisturizing cream
Diagnostics
The patient’s survey and examination data are usually sufficient to establish the diagnosis. In some cases, laboratory tests may be required to confirm the diagnosis.
Treatment
During the consultation, the treatment is selected for each patient individually, depending on the condition that caused the injury, concomitant diseases. In most cases, avoidance of factors that promote the appearance of the lesion is required.

Vitiligo – Why Do White Patches Appear on the Skin and How to Treat Them?
Vitiligo is a non-contagious skin condition characterized by white patches due to the loss of pigment. While it does not pose a direct threat to physical health, it can have a significant psychological impact. Learn what causes vitiligo, its symptoms, how it is diagnosed, and which treatment methods are currently available.
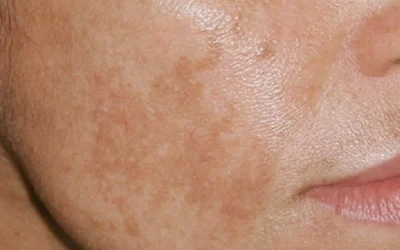
Hyperpigmentation: Causes, Types, and Modern Treatment Options
Hyperpigmentation is a common skin condition characterized by dark spots that appear due to sun exposure, hormonal changes, or skin damage. In this article, you will learn about the main types and causes of hyperpigmentation, as well as how to effectively treat it using modern dermatological methods and preventive care.
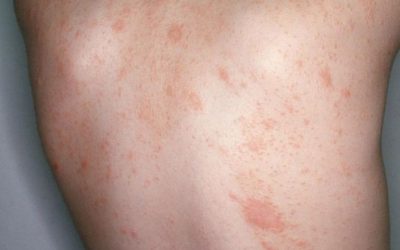
Pityriasis rosea
An acute, self-limiting, exanthematic skin disease that manifests as itchy, somewhat inflammatory, scaly rashes, usually on the torso, chest, and upper limbs.