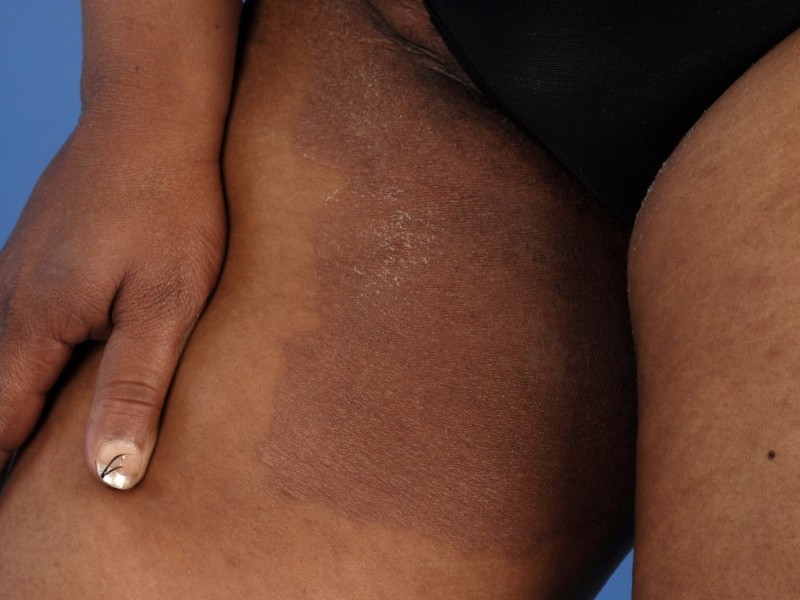
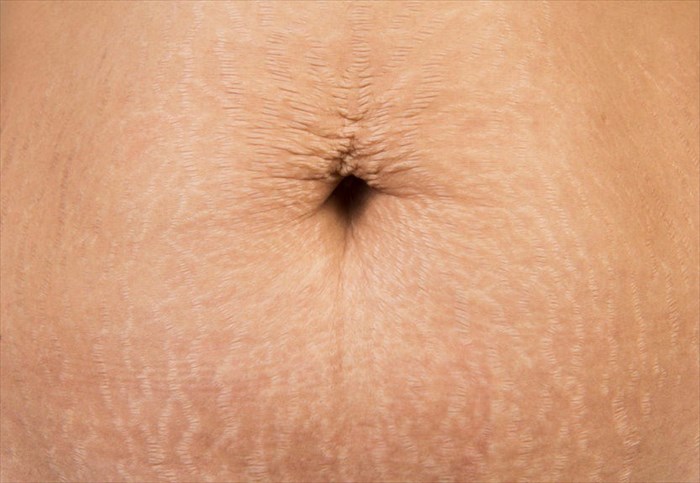
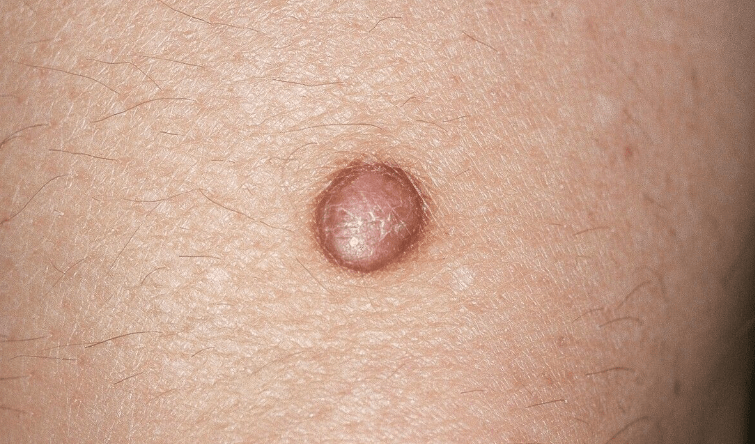
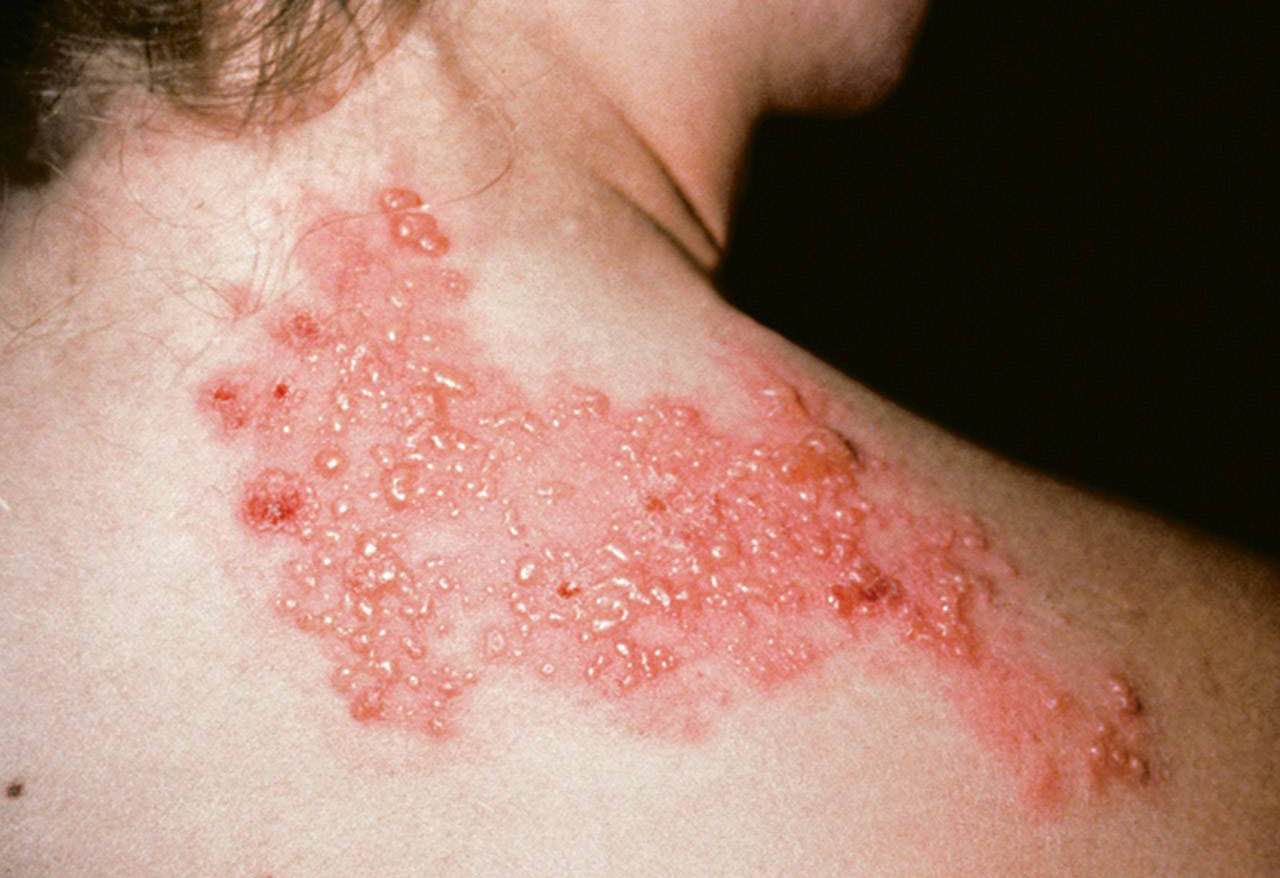
Shingles (Shingles)
iDermaThe team will provide a consultation within 24 hours, explain your skin assessment, and recommend the necessary treatment remotely!

If you are unsure about your skin concern and over-the-counter remedies are not helping, seek help from a dermatologist!