Psoriasis
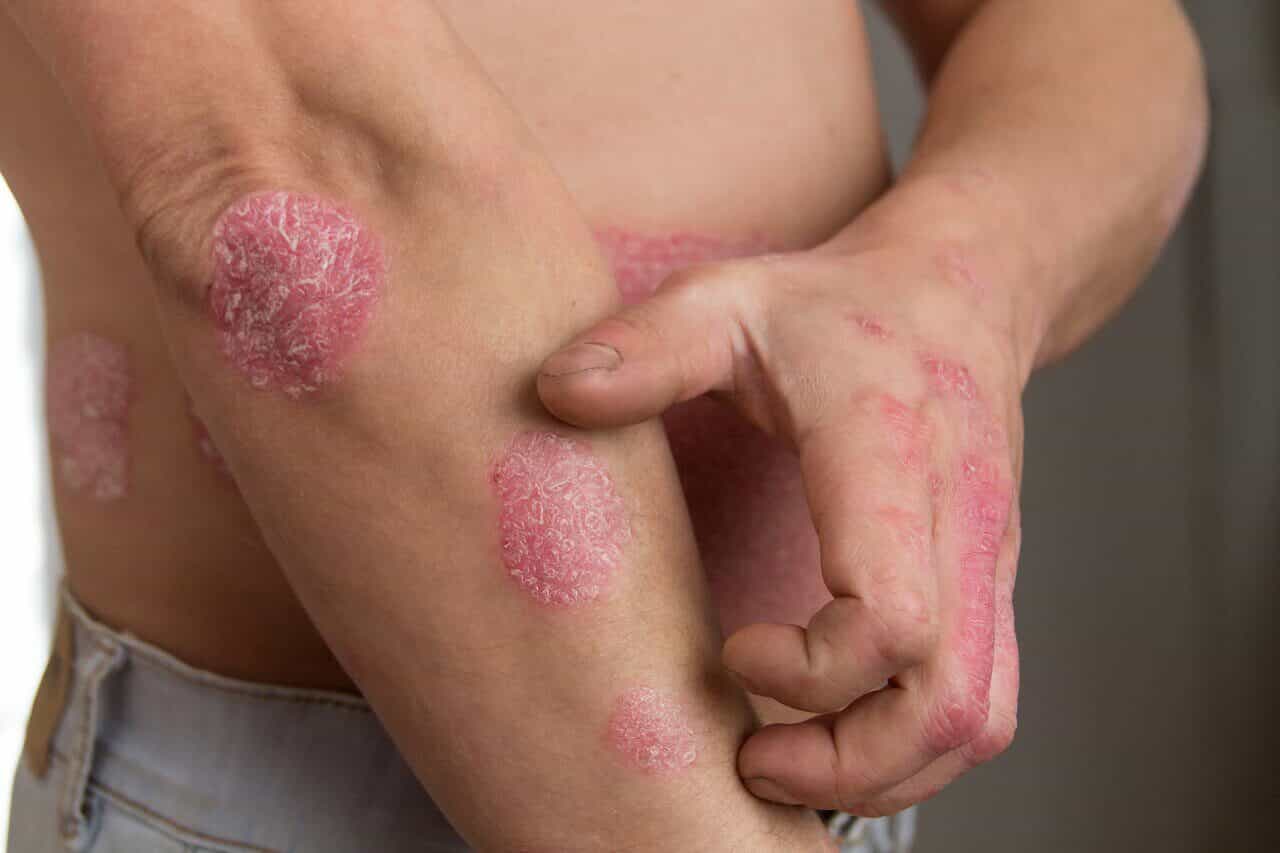
Psoriasis is a common chronic inflammatory skin disease affecting 2-4% of population with dermatitis.
-
- Psoriasis can start at any age, but it is most commonly diagnosed in adults (aged 30 to 39 and 50 to 69)
- Psoriasis incidence is the same in women and men
- Psoriasis is not an infection and is not contagious.
- Psoriatic arthritis is a common comorbidity of psoriasis
- The severity of psoriasis is determined by how much of the body’s surface is affected and how much the disease affects a person’s quality of life
- Psoriasis is an incurable disease but a very rare cause of death
Causes, risk factors
Scientists have not yet identified the exact cause of psoriasis, but it has been confirmed that the disease is caused by a combination of immune, genetic and environmental factors:
-
- Immune – the normal renewal of the skin layers is disrupted, immune cells stimulate the rapid proliferation of skin cells on the surface of the skin, and inflammation occurs.
- Genetics (40%) – heredity, i.e. a positive family history (e.g. close relatives – mum or dad, grandmother, etc.).
- Environmental factors such as bacterial and viral infections (e.g. HIV), smoking, alcohol consumption, stress, and certain medications (beta blockers, lithium, antimalarials) can all affect the risk of developing psoriasis, or worsen symptoms.
Genetic predisposition is considered a major risk factor, but environmental and behavioural factors can also influence the development and progression of psoriasis.
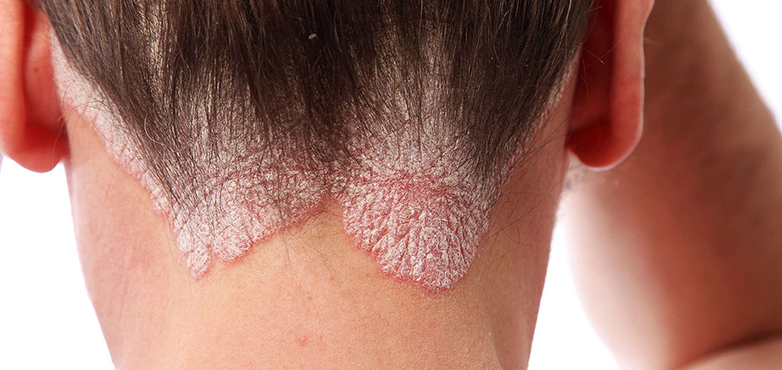
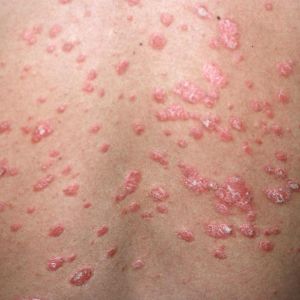
Types of psoriasis
Key:
-
- Plate (most common – 80%)
- Drip
- Half-empty
- Erythrodermic
Rarer, by body region:
-
- Body folds
- Nail
- Hands and soles
Symptoms
-
- Rashes may be visible on all areas of the body (except mucous membranes)
- Often spreading, merging
- Dry, red or dark-coloured skin lesions (papules, plaques, nodules, pustules)
- Rashes are usually covered with silver or white scales
- Nail abnormalities – may be discoloured, crusty, flaking, small pits may be visible (thimble phenomenon)
- Joint pain, stiffness (in psoriatic arthritis)
Diagnostics
-
- The diagnosis of psoriasis is made after an interview, a detailed life and medical history, and a physical examination (inspection, palpation of rashes). Scarring is characterised by the phenomenon of Auschwitz – a light scratching of the rash with a spatula reveals tiny droplets of blood)
- Skin biopsy in complicated cases
- No other laboratory tests to confirm the diagnosis
Additional assessment
-
- Patients with psoriasis are assessed for psoriatic arthritis, and if a lesion is suspected, radiological tests are performed and a rheumatologist is referred for consultation)
- Evaluate signs of other comorbidities (obesity, metabolic syndrome, hypertension, diabetes and atherosclerotic disease)
- Disease prevalence and severity are assessed using the Psoriasis Area and Severity Index (PASI)
- The quality of life of people with psoriasis is measured using a standardised questionnaire (Dermatology Life Quality Index, DLQI). People with psoriasis often feel very bad about their skin, and some experience depression or anxiety.
The most common diseases considered in the diagnosis of psoriasis are seborrhoeic dermatitis, chronic lichen planus, atopic dermatitis and monetic dermatitis, and less commonly subacute cutaneous lupus erythematosus, hairy erythematous dermatitis, scabies and cutaneous T-cell lymphoma.
Treatment
-
- Psoriasis is an incurable disease, but there are many treatments that reduce symptoms and improve skin condition
- Treatment depends on the severity of the disease, cost and convenience, and the person’s response to treatment
- Complex treatment is often recommended
- Scleroderma is treated with topical agents, systemic drugs, light therapy (phototherapy) and, less commonly, laser therapy
Advice
-
- If a similar rash appears, contact your doctor or dermatovenereologist for confirmation of the diagnosis and treatment.
- If you have been diagnosed with psoriasis, avoiding or eliminating risk factors is essential.
- Use the treatment as prescribed by your doctor.
- If you experience anxiety or depressive symptoms, tell your doctor or nurse, or contact a psychologist or psychotherapist.
- Use emollients (creams, ointments) every day, whether you use topical medicines or not. Moisturising creams with urea, salicylic acid, lactate or other keratolytic agents are most suitable. These substances have a moisturising and dandruff-flaking effect. It is usually advisable to apply the moisturiser before the medicine and let it soak in.

Vitiligo – Why Do White Patches Appear on the Skin and How to Treat Them?
Vitiligo is a non-contagious skin condition characterized by white patches due to the loss of pigment. While it does not pose a direct threat to physical health, it can have a significant psychological impact. Learn what causes vitiligo, its symptoms, how it is diagnosed, and which treatment methods are currently available.
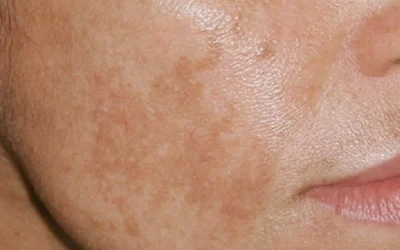
Hyperpigmentation: Causes, Types, and Modern Treatment Options
Hyperpigmentation is a common skin condition characterized by dark spots that appear due to sun exposure, hormonal changes, or skin damage. In this article, you will learn about the main types and causes of hyperpigmentation, as well as how to effectively treat it using modern dermatological methods and preventive care.
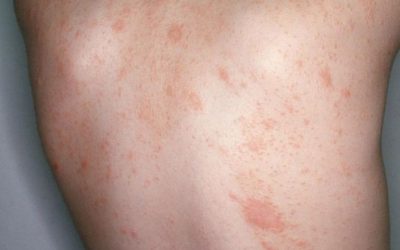
Pityriasis rosea
An acute, self-limiting, exanthematic skin disease that manifests as itchy, somewhat inflammatory, scaly rashes, usually on the torso, chest, and upper limbs.
iDerma
MB iDerma
Fabijoniškės g. 99, Vilnius
+370 670 70 822
info@iderma.lt